Wound care and vascular disease
Assessing wounds and vascular disease with transcutaneous oxygen measurement tcpO2
The value of oxygen in wound care
A wound is considered chronic if it doesn’t heal within four to six weeks and shows no signs of doing so. Chronic wounds are deficient in local oxygen, which is necessary for metabolism. [1, 2]
Patients with chronic wounds undergoing oxygen treatment may heal more rapidly as a wound heals faster in an oxygen-rich environment. [1, 2]


A type of vascular disease
The main risk factors of PAD are diabetes and smoking. More than 200 million people in the world live with PAD. [3, 4]
A possible complication to peripheral artery disease is the development of chronic wounds [1].
Lower extremity chronic wounds are challenging since wounds often do not respond to established medical procedures in a timely manner. Patients with chronic wounds present various local and systemic factors that can affect wound healing. As a result, patients with chronic wounds are at risk for lower limb amputation [5].
Critical limb ischemia
CLI is characterized by ischemic rest pain, ulcerations or gangrene. The circulation is so severely impaired that the patient is in imminent risk of limb loss without revascularization. [6]
The diagnosis of PAD is based on a clinical history-taking and a clinical examination, including the palpation of pulses and ankle brachial pressure index (ABPI) [6]. However, it has been suggested that performing pedal pulses is not enough to diagnose PAD in the diabetic population [15]. Furthermore, 1 out of 2 ABPI is highly elevated in diabetic patients [16].
Therefore, according to the Global Vascular Guidelines, the diagnosis of PAD should be done by performing ABPI, toe systolic pressure or transcutaneous oxygen tension [12].
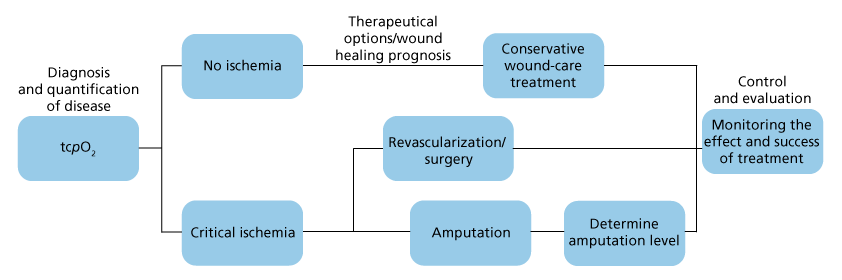
Treatment options
A frequently seen complication of diabetes is PAD which can lead to lower extremity ulcerations. Approximately half of all lower extremity amputations occur in patients with diabetes. [5]
Those who undergo lower extremity amputation experience:
- Increased healthcare costs
- A diminished quality of life [5]
The degree of ischemia needs to be assessed in order to determine the potential of wound healing. Treatment includes exercise, medical treatment, angioplasty and bypass surgery. If none of these options are sufficient for obtaining wound healing, amputation can be the last option. [6]
Assessing wound healing capacity and vascular disease
Transcutaneous monitoring can be used to indicate the likelihood of wound healing. In the cases of amputation, transcutaneous monitoring can provide supplementary information in the decision of appropriate amputation level [2, 5, 9, 10].
Tissue oxygenation measurements are adaptable as the heated, non-invasive sensors can be applied to different sites to create a perfusion map to better understand the patient’s wound healing potential [2].
Transcutaneous oxygen measurement (TCOM) or tcpO2 can predict the presence of vascular disease. It can thus be used to manage therapy. [9]
tcpO2 monitoring reference values
| tcpO2 < 30 mmHg | Insufficient for wound healing [7] |
| 30 mmHg < tcpO2 < 40 mmHg | Indicative of hypoxia [7] |
| tcpO2 > 50 mmHg | Average value of healthy subjects [7] |
Note: The range from 40 to 50 mmHg is considered a gray zone, where patients without comorbidities are likely to heal, whereas patients with comorbidities, such as diabetes and renal failure, are less likely to heal. [7]
TCOM and hyperbaric oxygen therapy
Transcutaneous oxygen measurement is widely used in hyperbaric oxygen therapy (HBOT) of wounds. It has gained importance as a tool for predicting potential candidates for hyperbaric oxygen therapy. [11]
The ability to increase the value of tcpO2 provides an indication of healing potential. The oxygen challenge aims to assess whether an increasing oxygen fraction in inhaled air results in an increased tcpO2 value. If positive, these patients are considered to benefit from HBOT. [7]
With patients breathing at their maximum amount, a tcpO2 value of > 100 mmHg indicates that macrovascular arterial disease is unlikely [7].
With hyperbaric oxygen therapy, a value of < 30 mmHg is consistent with severe arterial disease. A tcpO2 value > 35 mmHg indicates a likelihood of benefitting from HBOT. [7]
Initiating HBOT is the best way to assess if it's beneficial to a diabetic foot. A value greater than 200 mmHg is an indicator of successful healing. However, values of less than 100 mmHg are closely associated with the failure of HBOT. [7]




PeriFlux 6000 tcpO2 stand-alone transcutaneous monitor
The PeriFlux 6000 tcpO2 stand-alone transcutaneous monitor can support you in assessing patients with lower extremity wounds. By measuring trancutaneous oxygen in the tissue, you can measure the microcirculation of the patient's limbs.
Get a clear picture of a wound with information about the oxygenation levels of a patient's limbs.
References
- Barnikol W et al. A novel, non-invasive diagnostic clinical procedure for the determination of an oxygenation status of chronic lower leg ulcers using peri-ulceral transcutaneous oxygen partial pressure measurements: results of its application in chronic venous insufficiency. German Medical Science 2012; 10: 1-22.
- Padberg F et al. Transcutaneous oxygen (tcpO2) estimates probability of healing in the ischemic extremity. Journal of Surgical Research 1996; 60, 59: 365-369.
- Fowkes F et al. Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. The Lancet 2013; 382: 1329-40.
- Muntner P et al. Relationship between HbA1C level and Peripheral Artery Disease. Diabetes Care 2005; 28,8: 1981-87.
- Lo T et al. Prediction of Wound Healing Outcome Using Skin Perfusion Pressure and Transcutaneous Oximetry: a single-center experience in 100 patients. The Wound Treatment Center and Hyperbaric Medicine Service 2009; 21,11: 310-316.
- National Clinical Guideline Centre. Lower limb peripheral arterial disease, diagnosis and management, NICE Clinical Guideline 147. The National Clinical Guideline Centre, 11 St. Andrews Place, Regents Park, London NW1 4BT – United Kingdom, 2012.
- Fife CE et al. Transcutaneous oximetry in clinical practice: consensus statements from an expert panel based on evidence. University of Texas Health Science Center 2007; 36,1: 43-53.
- Norgren L et al. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). Eur J Vasc Endovasc Surg 2007; 33: 1-75.
- Bunt TJ et al. tcpO2 as an accurate predictor of therapy in limb salvage. Maricopa Medical Center 1996; 10, 3: 224-27.
- Kaur S et al. Evaluation of the efficacy of hyperbaric oxygen therapy in the management of chronic nonhealing ulcer and role of periwound transcutaneous oximetry as a predictor of wound healing response: a randomized prospective controlled trial 2012; 28,1: 70-75.
- Sheffield PJ. Measuring tissue oxygen tension: a review. Undersea Hyperbaric Medical Society 1998; 25,3: 179-188.
- Conte MS, Bradbury AW, Kolh P et al. Global vascular guidelines on the management of chronic limbthreatening ischemia. J Vasc Surg. 2019 Jun;69(6S):3S-125S.e40
- Hinchliffe RJ, Brownrigg JR, Apelqvist J et al. International Working Group on the Diabetic Foot. IWGDF guidance on the diagnosis, prognosis and management of peripheral artery disease in patients with foot ulcers in diabetes. Diabetes Metab Res Rev. 2016 Jan;32 Suppl 1:37-44.
- Hingorani A, LaMuraglia GM, Henke P et al. The management of diabetic foot: A clinical practice guideline by the Society for Vascular Surgery in collaboration with the American Podiatric Medical Association and the Society for Vascular Medicine. J Vasc Surg. 2016 Feb;63(2 Suppl):3S-21S.
- BBarshes NR et al. The system of care for the idabetic foot: objectives, outcomes and opportunities. Diabetic Foot & abjkem 2013.
- Portier et al. Use and Utility of Ankle Brachial Index in Patients with Diabetes. European Society for Vascular Surgery. 2010; 41:110-116
Cookies are used on this website
Use of cookiesPlease enter a valid email
We will be sending an e-mail invitation to you shortly to sign in using Microsoft Azure AD.
It seems that your e-mail is not registered with us
Please click "Get started" in the e-mail to complete the registration process
Radiometer is using Microsoft AZURE Active Directory to authenticate users
Radiometer uses Azure AD to provide our customers and partners secure access to documents, resources, and other services on our customer portal.
If your organization is already using Azure AD you can use the same credentials to access Radiometer's customer portal.
Key benefits
- Allow the use of existing Active Directory credentials
- Single-sign on experience
- Use same credentials to access future services
Request access
You will receive an invitation to access our services via e-mail when your request has been approved.
When you accept the invitation, and your organization is already using AZURE AD, you can use the same credentials to access Radiometer's customer portal. Otherwise, a one-time password will be sent via e-mail to sign in.